Blood glucose changes are not just influenced by food and medication; they can also shift with the seasons.
From colder, less active winter months to brighter, more active summers, changes in routine, diet, temperature, and even illness can all affect how your body manages glucose.
In this article, we explore why blood glucose changes throughout the year, what factors are behind these patterns, and practical ways to stay on track as the seasons change.
Contents
Changes in physical activity
Changes in diet and routine
Illness and infections
Temperature and insulin absorption
Medication and equipment factors
How seasons influence overall diabetes control
Spring and summer tips for managing blood glucose changes
Final thoughts on seasonal blood glucose changes
Changes in physical activity
One of the biggest seasonal influences on glucose levels is physical activity. During colder and darker months, people often move less, spend more time indoors, and exercise less frequently. Reduced physical activity can lead to higher blood glucose levels because muscles use less glucose for energy.
Diabetes UK notes that people often become less active during winter, which can make blood glucose levels rise and make diabetes harder to manage.
In contrast, warmer weather and longer daylight hours often encourage more outdoor activity, walking, and exercise, which can improve insulin sensitivity and help lower glucose levels.
Changes in diet and routine
Eating patterns often change with the seasons. Winter meals tend to be heavier and higher in energy, including dishes such as stews, pies, pasta bakes, and mashed potatoes. Festive periods can also lead to increased snacking, larger portions, and more alcohol.
These changes can influence glucose control. One study, Understanding temporal changes and seasonal variations in glycemic trends using wearable data, looking at people wearing Continuous Glucose Monitors (CGM), showed a noticeable drop in glucose control during the holiday period, highlighting how routine changes and celebrations can affect blood sugar levels.
During spring and summer, meals often become lighter and include more fresh vegetables and salads, which may contribute to improved glucose control.
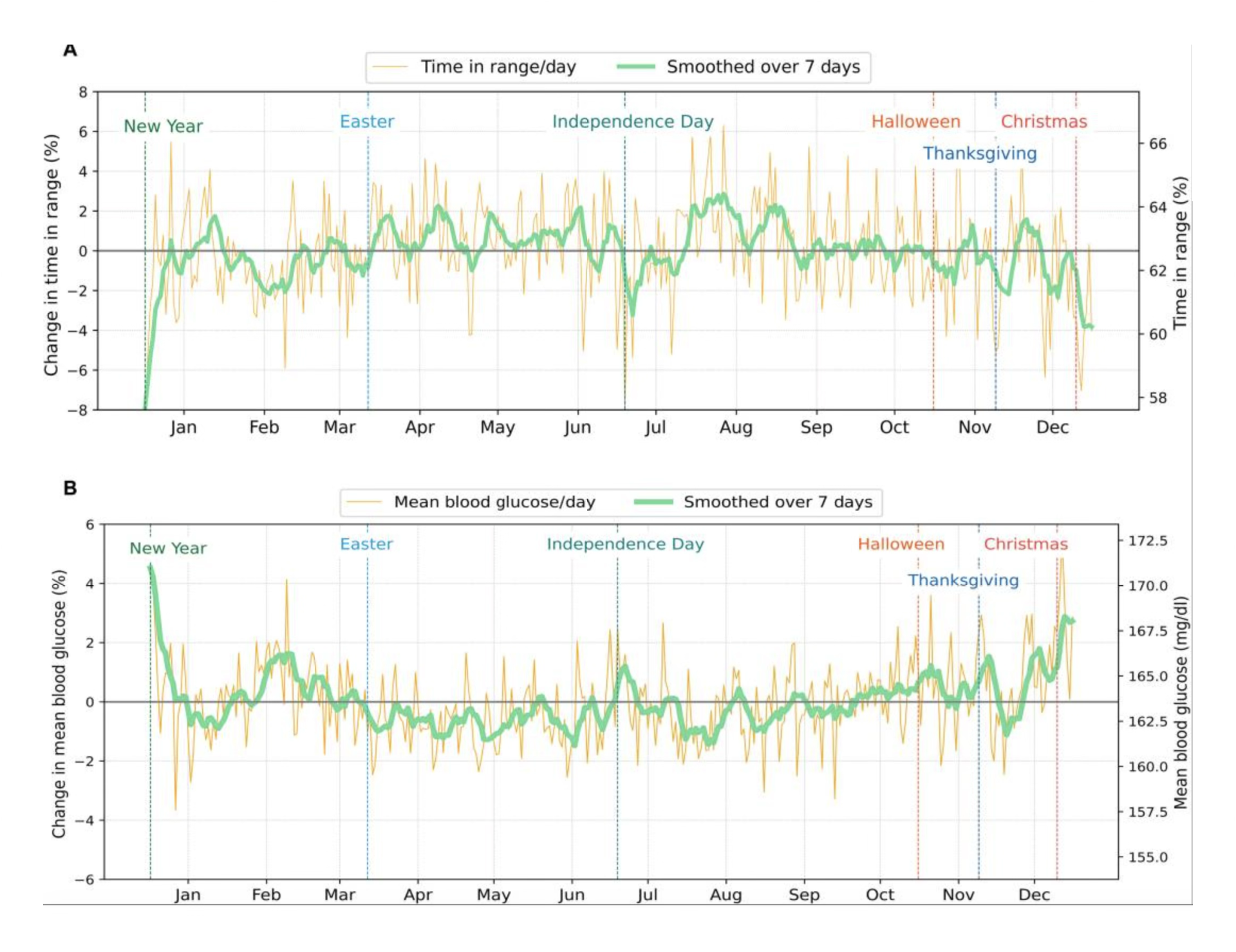
Fig. 2. The effect of holidays on glycemic trends in patients with diabetes. From Understanding temporal changes and seasonal variations in glycemic trends using wearable data.
Illness and infections
Respiratory infections such as colds and flu are more common in autumn and winter. Illness can significantly affect blood glucose levels.
When the body fights infection, it releases stress hormones that raise blood glucose. Diabetes UK explains that illness can cause blood sugar levels to rise even if someone is eating less than usual.
This means winter illness can temporarily make diabetes harder to control, particularly for people who use insulin.
Temperature and insulin absorption
Temperature can directly affect how insulin works in the body. Research has shown that warmer temperatures can increase insulin absorption from injection sites, meaning insulin may work faster in hot weather.
When warm temperatures are combined with exercise, insulin may be absorbed even more quickly, which can increase the risk of hypoglycaemia.
Hot weather can also increase fluid loss through sweating. Dehydration can concentrate glucose in the blood and make readings appear higher. Diabetes UK recommends staying well hydrated during warm weather and monitoring glucose levels more frequently.
Medication and equipment factors
Extreme temperatures can also affect diabetes equipment. Insulin that becomes too warm may lose effectiveness, which can lead to unexpectedly high blood glucose readings.
NHS guidance recommends storing unopened insulin in the refrigerator and keeping insulin, test strips, and glucose meters within recommended temperature ranges. Protecting diabetes equipment from excessive heat during summer and from freezing temperatures in winter helps ensure it works properly.
How seasons influence overall diabetes control
Seasonal changes can affect more than individual glucose readings. They may influence HbA1c levels, time spent within target glucose range, and the risk of hypoglycaemia.
A study examining people with type 2 diabetes found that achievement of treatment targets for HbA1c, blood pressure, and cholesterol was lowest during winter and highest during summer.
Winter can present several challenges at once. Reduced activity, increased illness, comfort foods, and disrupted routines may all contribute to slightly higher glucose levels.
Summer can bring its own challenges. Increased activity may improve glucose control but can also increase the risk of hypoglycaemia, especially in people using insulin or certain diabetes medications.
Spring and summer tips for managing blood glucose changes
Warmer months often bring more opportunities for outdoor activity, travel, and lighter meals. These changes can improve insulin sensitivity and help lower glucose levels, but they can also increase the risk of unexpected lows, particularly for people using insulin or medications that increase insulin production.
A few simple habits can help keep glucose levels stable during warmer weather.
Stay well hydrated
Hot weather increases fluid loss through sweating. Dehydration can make blood glucose appear higher because glucose becomes more concentrated in the bloodstream. Drinking water regularly helps maintain stable circulation and glucose levels.
Check glucose levels more frequently during heatwaves
Higher temperatures can increase insulin absorption, which may lead to faster drops in blood glucose. Monitoring more regularly can help identify patterns early.
Be prepared for increased activity
Longer days and better weather often lead to more walking, cycling, or gardening. Physical activity improves insulin sensitivity but may require small adjustments to carbohydrate intake or insulin dosing.
Protect insulin and diabetes equipment
Insulin can lose effectiveness if exposed to high temperatures. Keep insulin cool, avoid leaving it in direct sunlight or hot cars, and follow NHS storage guidance.
Plan ahead for holidays and travel
Changes in routine, meal timing, and activity can affect glucose levels. Packing snacks, checking glucose regularly, and keeping medication accessible can help prevent large swings.
Final thoughts on seasonal blood glucose changes
Scientific research shows that diabetes control often follows seasonal patterns. Blood glucose and HbA1c tend to be slightly higher during colder months and lower during warmer months, although the exact pattern varies between individuals.
These changes are influenced by multiple factors, including activity levels, diet, illness, temperature, and daily routines.
Recognising these seasonal influences can help people living with diabetes plan ahead, adjust their habits when needed, and maintain more stable glucose control throughout the year.
References
Higgins T et al. Seasonal variation in glycated haemoglobin in people with diabetes. Clinical Chemistry, 2009.
Mianowska B et al. Seasonal variation in HbA1c in children with type 1 diabetes. Diabetologia, 2010.
Belsare S et al. Seasonal and holiday patterns in glycaemic control from continuous glucose monitoring data. Science Advances, 2023.
Koivisto VA et al. Increased insulin absorption with rising ambient temperature. Metabolism, 1981.
Ronnemaa T et al. Exercise and warm temperature increase insulin absorption. Diabetes Care, 1988.
Sakamoto N et al. Seasonal variation in achievement of diabetes treatment targets. Diabetes Care, 2019.
Diabetes UK guidance on hot weather, cold weather, and illness.
NHS guidance on storing insulin.
Want to Learn More?
Grab a Copy of Carb & Calorie Counter
The multi-award-winning Carb & Calorie Counter book is your definitive, expert-approved guide to carb and calorie counting.
- Over 1700+ high-quality food photos
- Up to six portion sizes per food
- At-a-glance carbs and key nutrients
- The Original #1 Bestseller
With the “Carb-Counting Bible”, a single flick of the page is all you need to plan nutritious, carb-counted meals.


Contains hundreds of food photos that makes carb counting easy!
Sign up to the Carbs & Cals mailing list
Want to learn more about carb counting and the role of food in managing your health? Sign up to our mailing list!

