Ramadan is a deeply meaningful time of fasting, community and reflection for Muslims around the world. For people living with diabetes, fasting can present additional challenges, especially around blood glucose control, hypoglycaemia and meal planning.
This article gives an overview of UK-relevant advice to help you prepare safely for Ramadan, including when to avoid fasting, when you must break the fast, and practical ways to limit glucose spikes. Much of the guidance below is adapted from the South Asian Health Foundation Ramadan publication (2024).
Contents
A Reminder: Speak with your diabetes team before Ramadan
Who should not fast or consider not fasting for Ramadan
Ramadan fasting: When you must break your fast
Managing hypos and hypo symptoms
Medication and insulin considerations
Nutrition tips to limit blood glucose spikes
Low-Carb and Lower-GI choices
Tips to limit blood glucose spikes at Iftar
Physical activity and dehydration advice
The bottom line: Spiritual meaning and safe practice
A Reminder: Speak with your diabetes team before Ramadan
If you plan to fast, it’s important to have a pre-Ramadan review with your GP or diabetes specialist before the month starts. This allows you to:
- Assess your individual fasting risk.
- Personalise your medication or insulin plan.
- Review how you will monitor glucose safely during fasting hours.
This risk assessment may determine whether fasting is safe for you, or whether alternative acts of worship (like charity or fasting on shorter days) may be more suitable.
Who should not fast or consider not fasting for Ramadan
For some people, fasting may not be safe. It’s important to understand when the risks outweigh the benefits. You may be advised not to fast if you:
- Have Type 1 diabetes with frequent hypos or reduced hypo awareness.
- Have had a severe hypo or hospital admission for glucose issues in the last few months.
- Take insulin several times a day or use a mixed insulin regimen.
- Have an HbA1c that’s very high or diabetes that’s difficult to manage at the moment.
- Have diabetes complications such as kidney, heart or eye problems.
- Are pregnant, unwell or recovering from illness.
If any of the above apply to you, fasting can increase the chance of hypos, high glucose, dehydration or other complications.
Always speak to your diabetes team before Ramadan. They can help you understand your individual risk and guide you on what’s safe for you.
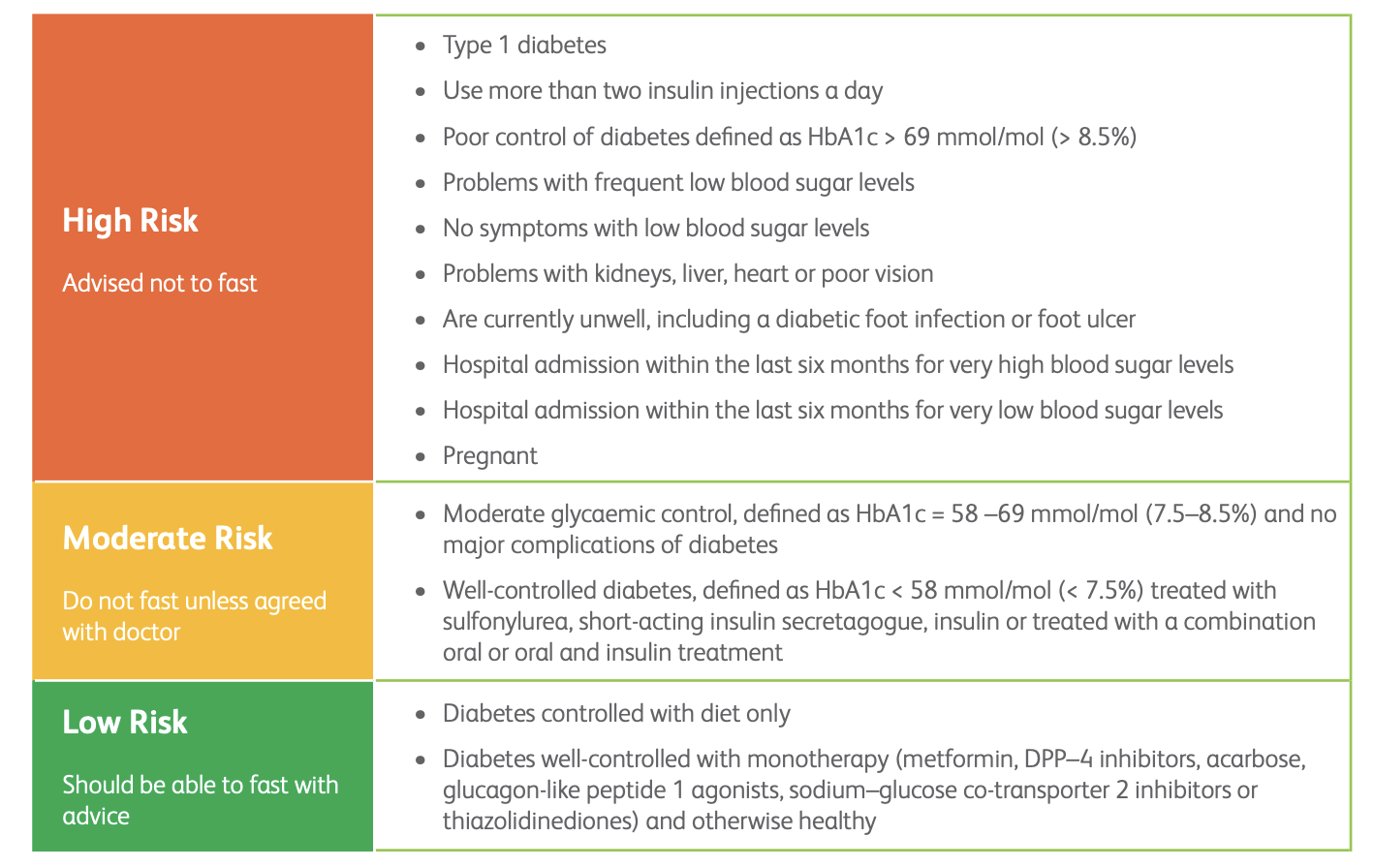
Table from the South Asian Health Foundation toolkit.
Ramadan fasting: When you must break your fast
The South Asian Health Foundation toolkit specifies the glucose thresholds and symptoms that mean fasting should be stopped immediately:
Break the Fast If:
- Blood glucose falls to ≤ 3.3 mmol/L at any time during the fast.
- You feel unwell or symptomatic of hypo (sweating, dizziness, confusion).
- Blood glucose is 3.9 mmol/L at the start of the fast and you take insulin or sulfonylureas.
- Blood glucose rises above 16.7 mmol/L.
- You show signs of dehydration (thirst, dizziness, dark urine, fatigue).
- You become disoriented, faint or unable to continue safely.
In all these cases, you should break your fast, treat as appropriate and ensure hydration and glucose stabilisation.
Monitoring does not break your fast
Testing blood glucose, whether finger-prick or CGM scan is allowed during fasting hours and is essential for safety.

Managing hypos and hypo symptoms
A “hypo”, blood glucose below 4.0 mmol/L, is a medical emergency during fasting and must be treated immediately:
- Use 15–20 g of fast-acting carbohydrate (glucose gel, juice, glucose tablets).
- Recheck after 10 minutes.
- Repeat if still low.
- Once stable, you may need to eat 15-20g of a slower a slower-acting carbohydrate to sustain levels.
It’s important to break the fast if hypos occur.

Medication and insulin considerations
Medication timing and dose can often need adjusting during Ramadan, depending on the type of medication you take. Each person’s regimen is different. A structured plan should be agreed with your healthcare team. Do not make changes unless you have been advised to do so by your healthcare team.
General Principles:
- Metformin can usually be continued at mealtimes.
- Sulfonylureas are more likely to cause hypos, dose timing or alternatives may be considered.
- DPP-4 inhibitors, GLP-1 receptor agonists, SGLT2 inhibitors typically have low hypo risk but hydration is important.
- Insulin regimens usually need thoughtful adjustment with your diabetes team.
Insulin Strategy
For many insulin users, the long-acting (basal) dose may be reduced and taken with Iftar, with bolus doses adjusted to Suhoor and Iftar carbohydrate content.
Nutrition tips to limit blood glucose spikes
During Ramadan, meals shift to:
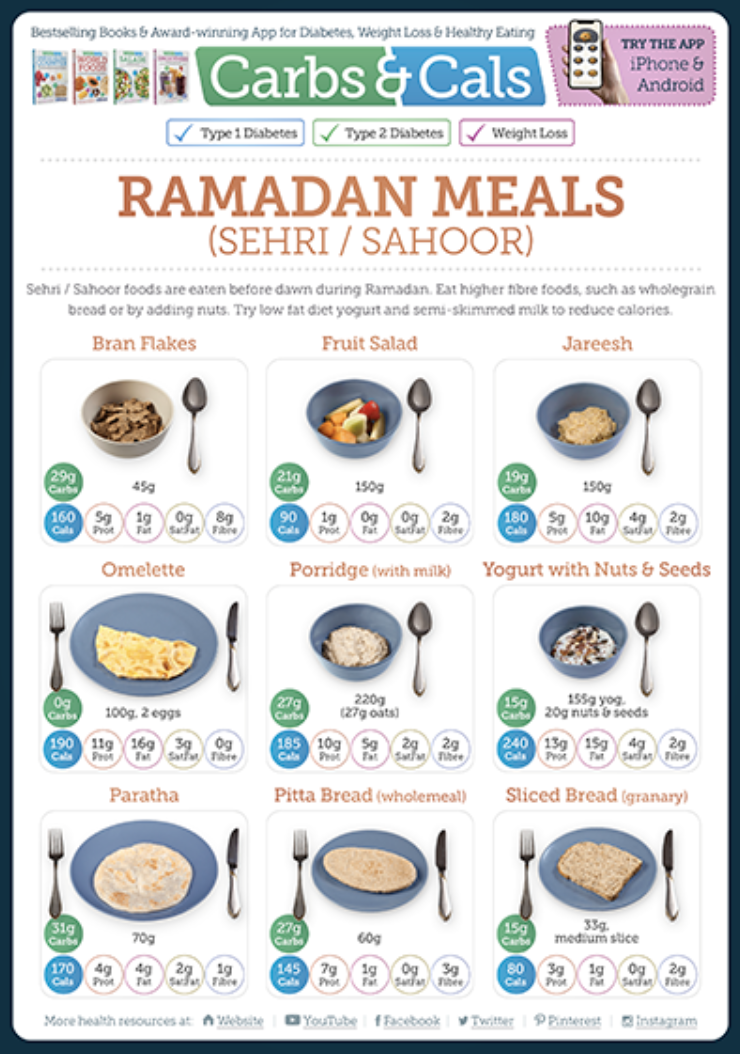
- Suhoor (pre-dawn meal): Often the key to stable glucose through the day.
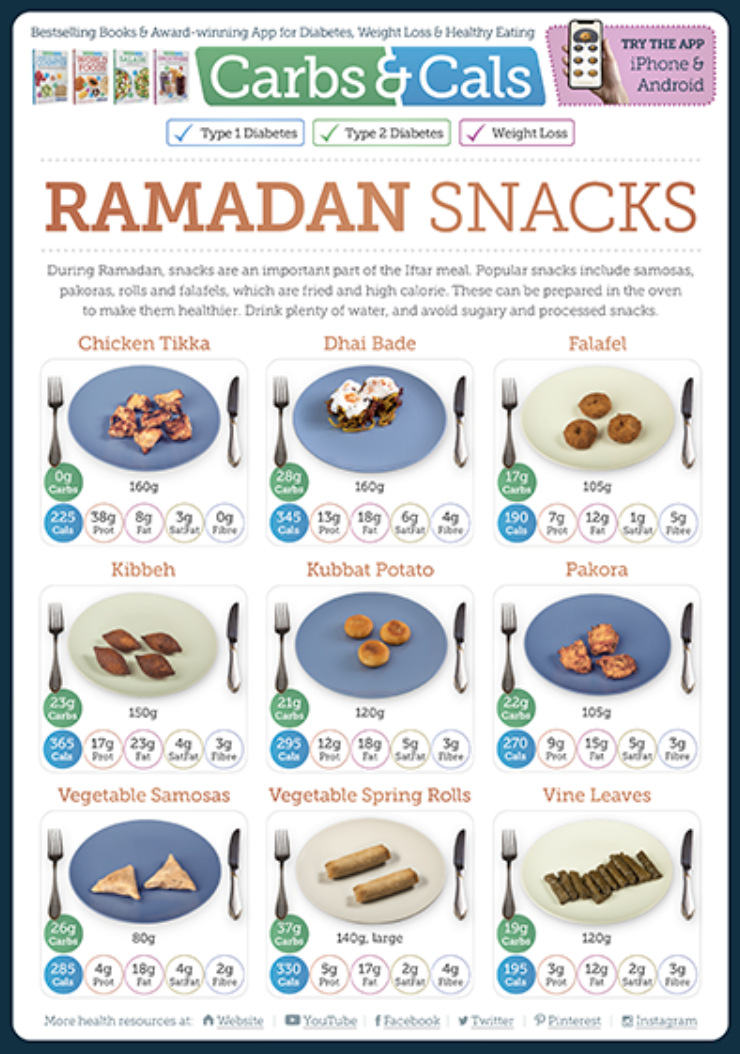
- Iftar (meal at sunset): Typically a larger meal and a time where rapid rises in blood glucose can occur if not managed carefully.
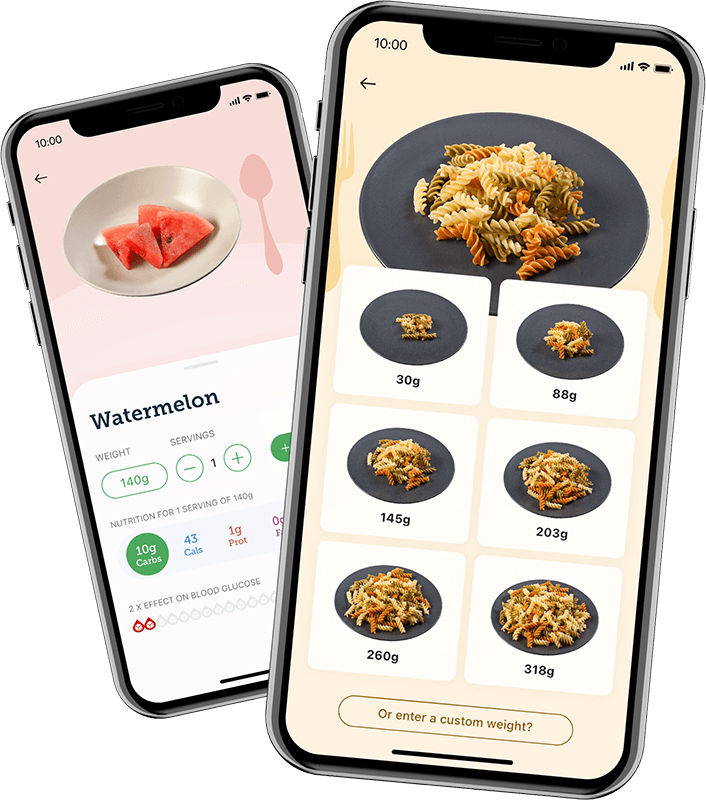
Carbs & Cals’ free Ramadan PDFs provide carb-counted portion photos for common Suhoor and Iftar foods, along with PDFs on breads, snack foods, sweets and drinks to help support your choices.
Low-Carb and Lower-GI choices
Choosing lower-glycaemic or lower-carb foods can help reduce post-meal spikes and keep you feeling fuller for longer.
Lower-GI options include:
- Wholegrains (bulgur wheat, wholemeal chapati, oats).
- Lentils, chickpeas (channa), beans.
- Non-starchy vegetables.
- Fruits such as apples, pears, berries.
Lower-carb swaps might include:
- Cauliflower rice instead of regular rice.
- Smaller portions of breads or rice balanced with more protein / veg.
- Using natural yoghurt, nuts or eggs at Suhoor for longer-lasting energy

Tips to limit blood glucose spikes at Iftar
The first meal after fasting can cause sharp rises in glucose, especially when foods are high in sugar or refined carbs.
Try:
- Opening Iftar gently, dates are traditional; stick to 1-2 small dates.
- Drinking water first to rehydrate.
- Avoiding large amounts of fried foods.
- Choosing wholegrain carbs where possible.
- Including lean protein (fish, chicken, eggs, beans).
- Adding fibre-rich vegetables to your plate.
- Eating slowly and avoiding oversized portions.
- If on rapid-acting insulin, discussing timing (often a pre-bolus can help) with your diabetes team.
Physical activity and dehydration advice
Exercise during fasting increases the risk of hypoglycaemia, especially for those on insulin or sulfonylureas.
- If you attend Taraweeh prayers, carry rapid-acting carbohydrate and water with you.
- Avoid intense exercise during fasting hours.
- Stay hydrated between Iftar and Suhoor to reduce risk of dehydration.
The bottom line: Spiritual meaning and safe practice
Many people with diabetes aim to fast during Ramadan, and with planning, individualised advice and self-monitoring, it can be done safely for some. But:
- Aim to have a pre-Ramadan health review.
- Understand your personal fasting risk category.
- Monitor glucose regularly during fasting periods.
- Plan out your meals and drinks to help limit blood glucose spikes and reduce the risk of dehydration.
- Break the fast if glucose thresholds or symptoms occur.
- Prioritise your health. Islam permits exceptions when fasting may harm you.
Other helpful resources:
Muslim Council of Britain Patient Information sheet: Ramadan and diabetes – A guide for patients
South Asian Health Foundation Patient Information sheet: Fasting with diabetes during Ramadan
Want to Learn More?
Grab a Copy of Carb & Calorie Counter
The multi-award-winning Carb & Calorie Counter book is your definitive, expert-approved guide to carb and calorie counting.
- Over 1700+ high-quality food photos
- Up to six portion sizes per food
- At-a-glance carbs and key nutrients
- The Original #1 Bestseller
With the “Carb-Counting Bible”, a single flick of the page is all you need to plan nutritious, carb-counted meals.


Contains hundreds of food photos that makes carb counting easy!
Sign up to the Carbs & Cals mailing list
Want to learn more about carb counting and the role of food in managing your health? Sign up to our mailing list!







